- ENVIRONMENTAL REMEDIATION- OIL WATER SEPARATORS
FREYTECH TECHNOLOGY INCREASES PRODUCTION AND REVENUE WHILE PROTECTING THE ENVIRONMENT IN 40 COUNTRIES AND COUNTING
ABOUT US
ECOSTORM is the Most Cost Effective Stormwater Filtration System on the
Market Today
LEARN MORE
SOME OF OUR PRODUCTS
-
Agricultural Soil Remediation, Disease Control & Crop Yield Augmentation
ButtonSolutions ranging from the repair and reclamation of degraded, damaged and over-farmed soil, through to maximizing crop yield.
-
Bee Colony Collapse Disorder (CCD) Remedy
ButtonEBD Systems are offered in a number of different configurations, shapes, sizes and materials to correct NEP (-) and PEP (+) imbalances in different environments and applications in order to resolve CCD.
-
Lake, River and Marine Algae Treatment
ButtonEBD Systems remediate rivers, lakes, wetlands and other bodies of water without using any of the costly conventional remediation methods which typically employ chemicals, filtration, retention ponds, dredging schemes, phytoremediation (plants), oxidation, non-indigenous bacteria etc.
-
EcoLine A
ButtonAbove ground oil water separation system to separate non-emulsified light liquids or low-water-soluble fluids with a specific gravity below 0.95 (gasoline, diesel, heating oils and other mineral oils) from effluent discharge.
-
EcoLine B
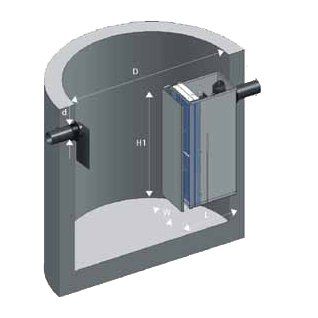
ButtonBelow ground oil water separation system to separate non-emulsified light liquids or low-water-soluble fluids with a specific gravity below 0.95 (gasoline, diesel, heating oils and other mineral oils) from effluent discharge.
-
EcoStop®
ButtonThe Ecostop Spill Control System with downstream automatic shut-off valve is designed to control spills at petroleum storage or fueling facilities.
-
EcoStorm Plus 400
ButtonAn affordable stormwater filtration system designed to remove sediments, heavy metals and nutrients from stormwater run-off. (100-175 sq. meter drainage area)
-
EcoStorm Plus 1000
ButtonAn affordable stormwater filtration system designed to remove sediments, heavy metals and nutrients from stormwater run-off. (500-1000 sq. meter drainage area)
-
EcoStorm Plus 1500
ButtonAn affordable stormwater filtration system designed to remove sediments, heavy metals and nutrients from stormwater run-off. (1000+ sq. meter drainage area)
-
XL Panels 40
ButtonDesigned to separate non-emulsified light liquids or low-water-soluble fluids with a specific gravity below 0.95 (gasoline, diesel, heating oils and other mineral oils) from effluent discharge.
-
EcoGrease
ButtonSystem to separate liquid, coagulating animal and vegetable fat and grease from water prior to discharge into septic or municipally owned sewers.
ECOSTOP is a One-of-a-Kind Patented Mechanical Inlet Oil Spill Prevention
Valve
LEARN MORE
NEWS